Peripheral Arterial Disease (PAD) is a condition that often goes undetected until symptoms affect daily life. Its impact on circulation can be serious, as restricted blood flow to the limbs can result in pain, numbness, and complications that interfere with mobility.
According to Konstantinos Marmagkiolis, advancements in diagnostic tools and minimally invasive treatments have improved prospects for those diagnosed with PAD, while changes in lifestyle like quitting smoking and adopting healthier habits play a crucial role in prevention and long-term care.
What is Peripheral Arterial Disease (PAD)?
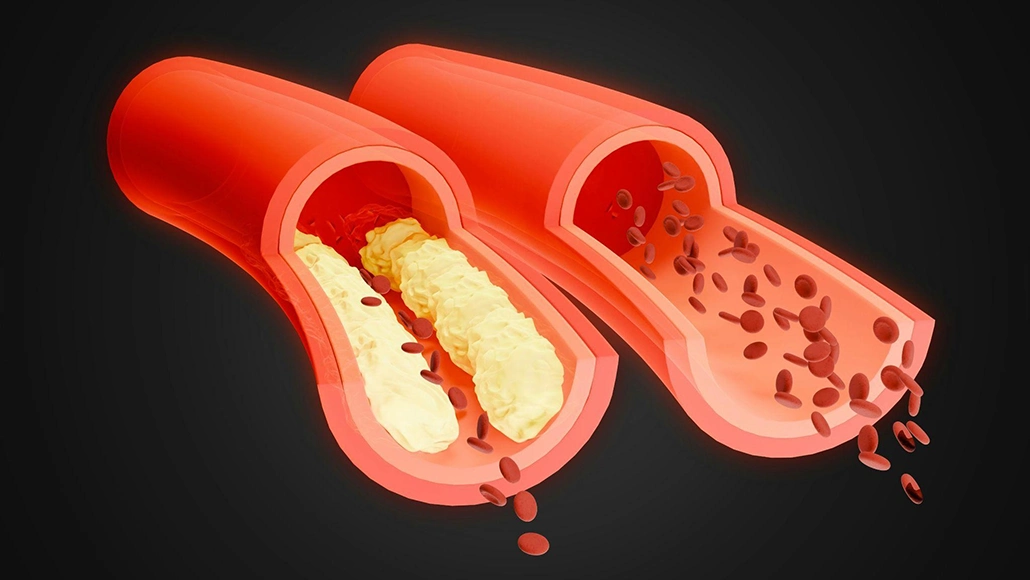
Peripheral Arterial Disease, or PAD, is a common circulatory disorder that happens when arteries supplying blood to the limbs become narrowed, most often due to a buildup of fatty deposits known as atherosclerosis. This restriction in blood flow primarily affects the legs, making it harder for oxygen and nutrients to reach muscles during activity.
People with PAD might notice that walking becomes difficult or uncomfortable, reflecting the underlying issue of reduced circulation. Everyday activities like climbing stairs or walking short distances may become increasingly tiring as the condition progresses. If left untreated, PAD can lead to more serious complications, including infections or even tissue loss.
Recognizing Key Warning Signs
One of the earliest signs of PAD is discomfort in the legs during physical activity, often described as cramping or aching that goes away with rest. Some notice persistent numbness, weakness, or a sensation of coldness in one leg compared to the other. In more advanced cases, wounds or sores may appear on the feet or toes that heal very slowly, if at all.
Persisting symptoms like these, especially in someone with risk factors, should prompt a conversation with a healthcare provider to rule out underlying vascular issues. Swelling or changes in skin color can also indicate compromised circulation, and recognizing these changes early can significantly improve treatment outcomes.
Risk Factors
Certain habits and health conditions can raise the likelihood of developing PAD, including smoking, diabetes, and high blood pressure. Age plays a role as well; those over 50 are more likely to experience symptoms. A family background of heart or vascular disease can also make someone more susceptible. Even high cholesterol levels or a sedentary lifestyle increase the risk, making it important to discuss these factors during regular medical checkups. Managing these factors and being aware of personal risk is vital for early detection and prevention.
How PAD is Diagnosed
Healthcare professionals often start with a physical exam, looking for signs such as weak pulses in the legs or changes in skin color and temperature. A simple test called the ankle-brachial index compares blood pressure in the ankle to that in the arm, helping to reveal any reduction in blood flow.
When further clarity is needed, imaging techniques such as ultrasound or specialized scans can provide a detailed view of the arteries, enabling a more precise assessment of blockages or narrowing. Sometimes, doctors may recommend additional blood tests or treadmill exercise tests to see how the legs respond to activity, which can provide further insight into the severity of PAD.
Examining Endovascular Solutions
Treatments for PAD have advanced, with endovascular procedures offering less invasive ways to restore blood flow. Angioplasty and stent placement are two common methods where a small balloon or mesh tube is used to open narrowed arteries, providing relief from symptoms. In certain cases, atherectomy might be performed to remove plaque buildup directly from the artery wall.
These usually mean a shorter hospital stay and quicker return to daily activities, though careful follow-up is important to ensure long-term success. Sometimes, medications to prevent blood clots or manage cholesterol are prescribed alongside these interventions, further improving outcomes.
Preventive Strategies and Lifestyle Adjustments
Taking steps to reduce risk factors makes a significant difference in managing PAD. Quitting tobacco, staying physically active, and choosing heart-healthy foods support better circulation and overall health. Monitoring conditions like diabetes and high blood pressure can limit further artery damage, making regular medical checkups a wise investment in long-term well-being. Making these changes can help slow the progression of PAD and improve quality of life.