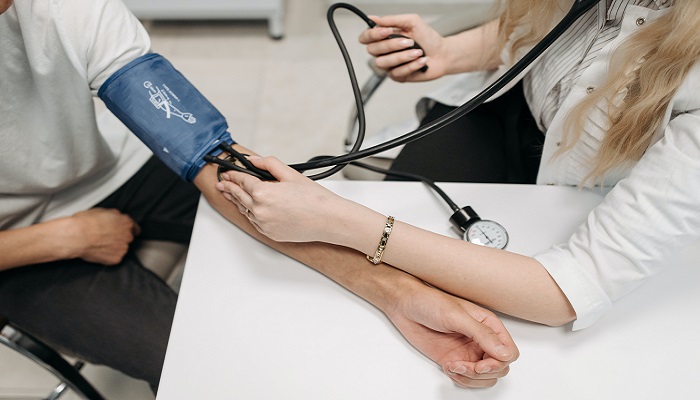
Managing, mitigating, and mastering chronic disease care in family medicine clinics is no small task, but with the right strategies, you can make it more manageable.
This guide offers an overview of best practices to ensure optimal care for patients dealing with chronic illnesses. We’ll delve into the importance of early detection, patient education, and engagement, as well as the role of multidisciplinary teams and health technology.
You’ll also learn about personalizing treatment plans, continual patient monitoring, and fostering healthy lifestyle changes.
Understanding Chronic Diseases
Chronic diseases are long-term medical conditions that, despite often being manageable, have no current cure. These illnesses, like diabetes, heart disease, or arthritis, impact your life daily and require continuous medical attention.
You’re not fighting a temporary battle, but learning to coexist with a persistent condition.
You must understand your illness to manage it effectively. That’s why you should constantly communicate with your healthcare provider, ask questions, and follow the care plan agreed upon.
Also, lifestyle modifications, such as healthy eating and regular exercise, can significantly help in managing the symptoms.
The Importance of Early Detection
Early detection increases the chances for successful treatments, reduces the risk of complications, and can significantly improve your quality of life.
Regular check-ups and screenings in a clinic or medical center are essential tools for early detection. These simple steps can identify potential health issues before they become severe or even life-threatening.
If you’re at risk for certain conditions, such as diabetes or heart disease, it’s crucial to discuss this with your healthcare provider. They can guide you to the appropriate screenings or tests.
Patient Education and Engagement
The next crucial step in managing chronic disease is your active involvement and understanding of your condition, which can be achieved through patient education and engagement.
This requires you to:
- Actively participate in your care by asking questions and seeking clarity about your condition.
- Regularly follow-up with your healthcare provider to monitor your progress and adjust treatment as needed.
- Proactively manage your lifestyle, including diet, exercise, and stress levels, to support your overall health.
Multidisciplinary Care Teams
Multidisciplinary care teams play a pivotal role in your chronic disease management, offering a diverse range of expertise and perspectives for more comprehensive and effective patient care.
This team could include doctors, nurses, dieticians, physiotherapists, pharmacists, and social workers, all working together to provide cohesive care. These professionals pool their knowledge to address your unique health needs.
For example, a dietician can help manage your diabetes with diet, while a physiotherapist can provide exercises to keep you active and healthy. This collaborative approach ensures you receive well-rounded care, tailored to your specific conditions.
Utilizing Health Technology
Another critical aspect of chronic disease care is the effective use of health technology. As a caretaker, you should be utilizing tech advancements to enhance patient care.
Here are four key strategies:
- Use Electronic Health Records (EHRs) to keep track of patient history and improve diagnostic accuracy.
- Implement telemedicine when possible to give patients with mobility issues access to care.
- Employ predictive analytics to anticipate and prevent disease flare-ups.
- Use digital signs to offer personalized patient education, self-management tips, and targeted infotainment to improve health outcomes and engagement of patients with chronic disease.
Integrating these technologies not only improves the quality of care but also helps patients manage their conditions more efficiently.
Personalizing Treatment Plans
As a healthcare provider, you need to recognize that no two patients are alike, and because of this, each individual’s treatment plan should be tailored to their unique needs and circumstances.
This personalization might involve considering their age, lifestyle, other existing health conditions, and their personal preferences.
You’ll need to communicate effectively, involving patients in decision-making and ensuring they understand their options. It’s also crucial that you monitor the impact of the treatment regimen and adjust it as necessary.
While implementing personalized treatment plans requires more time and effort, it can lead to improved patient outcomes and satisfaction.
Continual Patient Monitoring
Patient monitoring is a cornerstone of effective chronic disease care in your family medicine practice. It’s not only about diagnosing and treating, but also keeping a close eye on your patient’s health status over time.
Here’s a simple guide to make it work:
- Schedule routine appointments to evaluate the patient’s condition and make necessary adjustments to the treatment plan.
- Incorporate telemedicine and wearable devices for real-time health tracking. This can provide valuable data and alert you to any sudden changes.
- Empower patients with knowledge about their condition. Encourage them to report any symptoms or concerns promptly.
Fostering Healthy Lifestyle Changes
Fostering healthy lifestyle changes in your patients as part of their chronic disease management is also essential. But how do you do this effectively?
- Start by introducing small, manageable changes.
- Encourage regular exercise, even if it’s just a short walk around the block.
- Advocate for a balanced diet, rich in fruits, vegetables, and lean proteins.
- Emphasize the importance of adequate sleep and stress management techniques.
Remember, it’s not about overnight transformation, but gradual, sustainable change. You’re not just treating symptoms, you’re helping to reshape habits.
Conclusion
Caring for long-term illnesses like diabetes or heart disease in family clinics involves teamwork, smart planning, and listening to what patients need. It’s important to catch diseases early through check-ups, and patients should learn about their health condition to help manage it.
Healthcare workers like doctors, nurses, and dietitians work together to offer the best care tailored to each person.
Using technology like online medical records and health tracking apps can improve care.
Treatment plans should be customized, and keeping a regular check on the patient’s health is necessary.
Lastly, encouraging small but important lifestyle changes, such as more exercise and eating healthy, can have a big impact on health.
Everyone’s effort counts when it comes to managing chronic diseases, and small steps can lead to big health gains.
FAQs
What is the role of primary care physicians in managing chronic disease?
Primary care physicians are pivotal in diagnosing, orchestrating treatment plans, and coordinating ongoing care, often collaborating with specialists to ensure that patients’ chronic conditions, such as diabetes or heart disease, are managed effectively to improve their quality of life and prevent complications.
What is the most common disease in family medicine?
Hypertension, or high blood pressure, frequently tops the charts as the most common disease encountered in family medicine. It’s a silent predator, often presenting few symptoms but leading to serious heart risks if left unchecked.
What is the hardest chronic illness to live with?
The hardest chronic illness to live with is subjective, as it can vary widely from person to person based on factors like severity, personal circumstances, and the effectiveness of treatment. Diseases like Chronic Obstructive Pulmonary Disease (COPD), chronic pain conditions, and autoimmune diseases like lupus often rank highly for their impact on daily living and the challenges they pose for both patients and caregivers.
What is a chronic disease clinic?
A chronic disease clinic specializes in the comprehensive management of long-term illnesses. These clinics offer a coordinated approach, often involving a team of specialists who work together to provide tailored care, education, and support for individuals with enduring conditions such as diabetes, arthritis, or heart disease, helping them navigate the complexities of their illness.