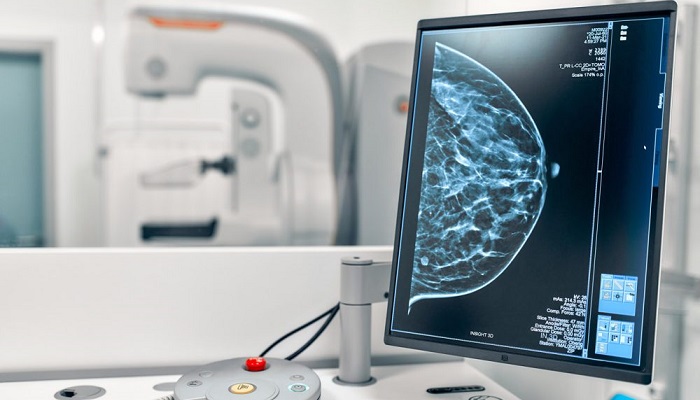
Breast cancer happens to be one of the leading causes of cancer death in women. Around 47% of women across the US have dense breasts, which is one of the independent risk factors as far as breast cancer is concerned. Apparently, women who have dense breasts have a high amount of fibrous connective and glandular tissues and low amounts when it comes to fatty tissues.
Although screening mammography precisely detects almost 98% of cancer in fatty breasts, breast cancer largely gets missed when it comes to dense breasts. This goes on to show a negative mammogram, thereby giving false reassurance to patients. As per the study’s co-author, Dr. Vivianne Freitas, MD ad M.Sc. from the university of Toronto, the breast cancer masses appear white on a mammogram, and even the dense tissues appear to be white, which makes finding breast cancer in a patient with dense breasts significantly harder.
Additional screening may thereby be required in order to assist cancer detection in women who have dense breasts. The four most general supplemental breast tests are automated breast ultrasound, hand-held breast ultrasound, breast MRI, and digital breast tomosynthesis. According to Dr. Freitas, their study was meant to analyse the role of every supplementary screening test in any woman who has an intermediate breast cancer risk, has dense breast tissue, and has also had a negative mammogram.
To evaluate which screening method was perfect to those with dense breasts, scientists conducted a meta-analysis on around 22 studies which had 261,233 patients being screened for breast cancer. While ten studies focused on hand-held breast ultrasound, four covered automated ultrasound, eight studies took digital breast tomosynthesis into account, and three covered breast MRI. Of all the individuals who were screened, 132,166 patients had a negative mammogram but dense breasts. In order to identify patients who have an average or intermediate risk of developing breast cancer, risk assessment models have been taken into account. It is well to be noted that the women in the US with a lifetime risk estimation of 12 to 13% of breast cancer development are considered to have an average risk. Elements that elevate the risks to intermediate have a breast cancer treatment history or previous breast biopsies. High-risk patients having a lifetime risk of 20% or even higher were excluded from the study as the breast MRI benefit was already established across high-risk populations.
Meta-analysis showed that from 132,166 patients who had dense breasts, 541 breast cancers got missed on mammography initially and were detected via supplemental methods of screenings. Breast MRI was a superior screening method and could detect even the smallest of cancers. Dr. Freitas added that MRI happens to be a far more superior method when it comes to cancer detection as compared to other sources. It is well to be noted that the results on the MRI’s role when it comes to supplementary screening will help stakeholders guide healthcare policies and also direct further research.
Although the study lays out the effectiveness of breast MRI when it comes to cancer detection, there is still a requirement for more research. According to Dr. Freitas, before one can advocate for wider MRI application in women, an analysis of its cost effectiveness compared to other techniques, its role in reducing mortality, etc. will have to be studied. At this point in time, as per her, the cost of the breast MRI as well as its availability can be seen as the biggest hurdle in its widespread implementation.