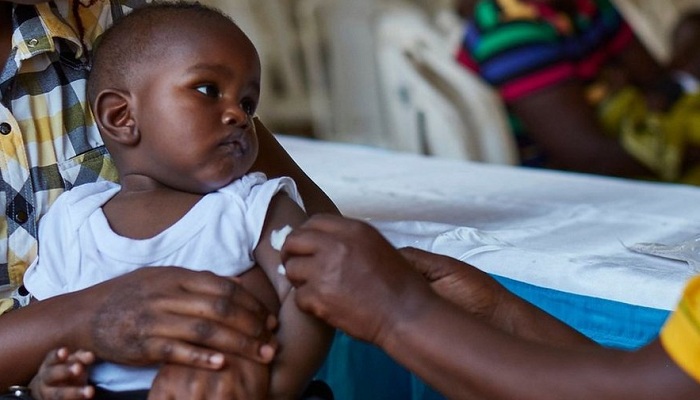
More than a million children in Ghana, Kenya, and Malawi have been given one or more doses of the world’s first malaria vaccine, owing to a pilot programme supervised by WHO, as World Malaria Day approaches this year. The RTS,S/AS01 (RTS,S) vaccine is feasible and safe to deliver, and it significantly reduces lethal severe malaria, as per the malaria vaccine pilots, which were first launched by the Malawian government in April 2019.
These findings helped pave the way for the historic WHO recommendation in October 2021 to expand the use of RTS,S in children residing in neighbourhoods where malaria transmission is relatively high. WHO believes that if the vaccine is widely used, it will save the lives of an estimated 40 000 to 80 000 African children per year.
Gavi, the Vaccine Alliance, has pledged more than US $155 million to support the launch, acquisition, and distribution of the malaria vaccine in Gavi-eligible nations in Sub-Saharan Africa. Countries can get advice from WHO on whether and how to use RTS,S as a supplementary tool to reduce malaria-related illness and mortality in children. As a malaria researcher in his early career, he dreamt of the day humanity would have an effective vaccine against such a dreadful illness, said WHO Director-General Dr Tedros Adhanom Ghebreyesus. This vaccination isn’t only a scientific triumph; it’s a game-changer for African families. It exemplifies the importance of science and advancement in the field of health. Nonetheless, new and better instruments are urgently needed to save lives and enhance performance toward a malaria-free future.
New intervention possibilities
RTS,S is a first-generation vaccine that may be supplemented by additional vaccines with similar or higher efficacy in the future. The World Health Organization praises the progress made in the area of R21/Matrix-M as well as other malaria vaccine alternatives in treatment trials. Clinical studies for these vaccines must be successfully conducted in order to determine their safety and effectiveness characteristics. WHO also praises BioNTech’s announcement that it plans to create a malaria vaccine using mRNA technology. BioNTech is the maker of the Pfizer-BioNTech COVID-19 vaccine.
A variety of novel instruments and methods in the realm of vector control have been presented to WHO for review. If they prove successful at managing chronic diseases, WHO will issue new recommendations or change current ones to boost their use. New forms of insecticide-treated netting, spatial insect repellents, gene-drive techniques, and sugar baits to lure and kill Anopheles mosquitoes are just a few examples.
In addition, there are other novel drugs in the works. WHO commends the Australian Therapeutic Goods Administration’s recent clearance of dispersible single-dose tafenoquine tablets for the control of P. vivax malaria in children. The US Food and Drug Administration, as well as drug regulatory agencies in other countries such as Brazil, Peru, and Thailand, have all authorised tafenoquine for use in adults. Tafenoquine is predicted to ensure better adherence to therapy when given as a single dosage. A 7-to-14-day course of medicine is the normal version of therapy.
For the treatment of simple and serious malaria, a variety of additional antimalarial drugs with new mechanisms of action are being developed. The first non-artemisinin combination medication, Ganaplacide-Lumefantrine, is currently in a Phase II clinical trial and could be useful in the fight against drug-resistant malaria in Africa. In addition to drug resistance, WHO has identified other serious threats to malaria control, which include insecticide-resistant mosquitos, an invasive malaria vector that thrives in both urban and rural locales, and the rise and scatter of mutated P. falciparum parasites that are compromising the accuracy of rapid diagnostic tests. To fight these threats, new tools and methods will need to be used, with a more strategic use of existing tools.
More funds are needed
Global progress in lowering malaria incidence and fatalities has slowed or stagnated in recent years, as per 2021 World Malaria Report, specifically in countries hardest afflicted by the disease. The report highlights the importance of continuing innovation in research into new instruments if the world is to reach the WHO malaria strategy’s 2030 targets.
In 2020, funding for malaria research and development was just over US $619 million. In the decade 2021–2030, an average annual R & D investment of US $851 million will be required.
Getting the most out of what we have, already
To meet global malaria targets, innovative methods for the use of already existing instruments will be required. Nations hit hardest by malaria have been gathering and processing malaria data to better understand the disease’s geographical spread thanks to WHO and the RBM Partnership to End Malaria’s “High Burden, High Impact” approach, which was launched in 2018 by WHO and the RBM Partnership to Wrap Up Malaria.
They are investigating the potential impact of customised bundles of treatments guided by local data and the local disease situation, rather than taking the same strategy for malaria control everywhere. These studies will enable governments to make more effective, efficient, and equitable use of available money.
RTS,S malaria vaccine and pilot programme
Countries can now get WHO recommendations on whether and how to incorporate the RTS,S vaccine into their malaria control plans. The vaccine has recently been added to WHO’s unified malaria recommendations, and WHO has also released an amended policy statement on the vaccination. The vaccine has been favourably received by African communities in routine usage to date. The current vaccine manufacturing capacity is capped at 15 million doses per year, but demand is expected to surpass 80 million doses per year.
Increased manufacturing capacity of RTS,S and acceleration of the production of other first-generation and next-generation malaria vaccines are two ways WHO is working with partners to improve supply. WHO is coordinating the creation of a framework for the allocation of limited malaria supply to guide where initial doses of the vaccine will be deployed; the goal is to prioritise areas of high need and greatest malaria burden until supply matches demand.
The RTS,S pilot programme is made possible by unparalleled partnerships between in-country and foreign organizations, including the Ministries of Health of Ghana, Kenya, as well as Malawi; in-country evaluation partners such as PATH, GSK, UNICEF, and others; and Gavi, the Global Fund, and Unitaid funding bodies.
GSK spent 30 years researching and developing the RTS,S malaria vaccine, which was made possible by cooperation with PATH and a chain of African research institutes.