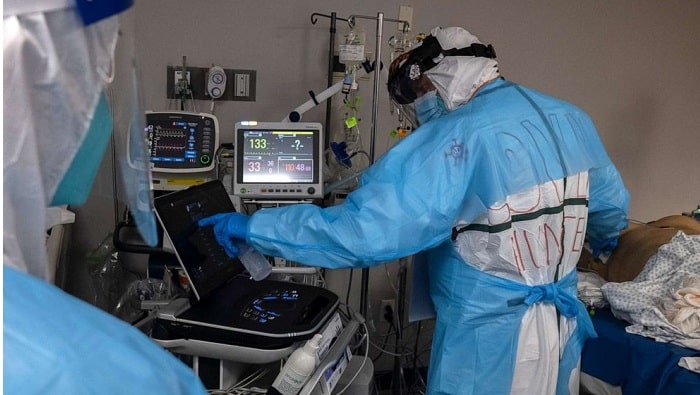
In the smaller towns in Texas, where cars are sometimes outnumbered by friendly animals roaming the neighborhoods, COVID-19 is still a concern.
Places like El Paso and the Texas Panhandle have seen recent surges in COVID-19, causing stress on the hospitals in those areas. So much so that Austin Mayor Steve Adler said last week that Austin was taking in non-COVID patients from El Paso.
“The entire year has been all COVID, all the time,” said John Henderson, the president and CEO of the Texas Organization of Rural and Community Hospitals. “But somewhat uneven, where we see these unpredictable regional flare-ups. More recently, it’s been the western and northwestern half of the state just covered up with COVID and struggling to staff and care for the patient load that we’re experiencing currently.”
He added that Central Texas’ rural hospitals are OK for now, but continued to warn that COVID-19 case numbers are heading in the wrong direction.
“So, it might just be a matter of weeks before they’re in a situation like the Panhandle or far West Texas is currently,” Henderson said. “The Central Texas rural hospitals are not immune to this. They will feel it until we can get the thing under control or the vaccine gets distributed broadly.”
Henderson explained that the Texas Organization of Rural and Community Hospitals typically exists to advocate for the needs rural hospitals have. But the organization has taken on an extra role in helping to provide personal protective equipment (PPE).
“We don’t normally procure and distribute supplies, but, you know, 2020 has been anything but a normal year,” Henderson said. “So, we’ve kind of jumped into that, just trying to help.”
He also explained that he would not say PPE is at the top of the list of concerns anymore for rural hospitals that are struggling, and that it’s more so issues pertaining to staffing and logistics.
“They’re dealing with COVID outbreaks among their nursing staff and struggling to staff the hospital,” Henderson said. “And then the other is patient transfers. So, when patients need a higher level of care or surgical intervention or an ICU bed, normally, it’s the rural hospitals that transfer those patients to the urban hospitals. Right now, they’re having trouble arranging those transfers because the urban hospitals are feeling such, such a load from COVID.”
“A lot of rural hospitals simply don’t have ICU beds or event capacity, and that’s why they’re trying to stabilize and transfer currently. Some do have that capability, but regardless, they’re all really being stretched to the limit this week,” he said.
Dr. Diana Fite, the president of the Texas Medical Association, elaborated on Henderson’s explanation of staffing problems in some rural hospitals.
“Ironically, sometimes the large city hospitals are transferring to the rural hospitals, just trying to find a place to put a patient in ICU. But the problem with the rural hospitals, the intensive care units are very small. They may have four beds, six beds, eight beds at the most,” Dr. Fite said. “And so, all you need is just a few patients to fill that up. Plus, the staff is a concern. If you have a few of the staff that get sick and have to quarantine out, then you don’t have enough staff to take care of those patients either.”