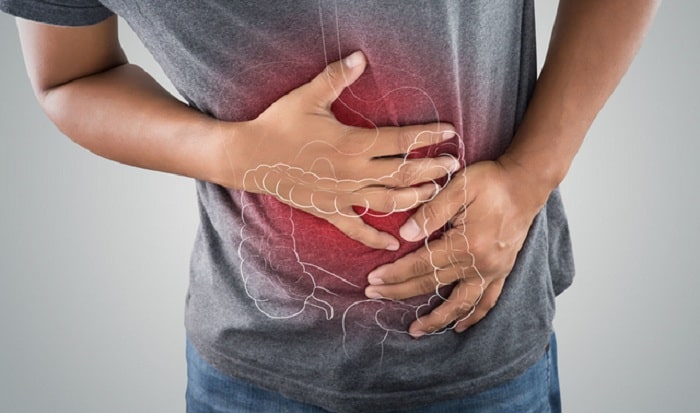
Crohn’s disease is a chronic gastrointestinal condition that causes inflammation of your digestive tract. It’s one of the most common forms of inflammatory bowel disease (IBD). Crohn’s-related inflammation causes a variety of symptoms, and common among them is constipation.
Sometimes, a person’s IBD constipation might persist even when their IBD treatment plan is in sustained remission, minimizing or even eliminating other Crohn’s symptoms. Because of this, it can be especially helpful to understand how to manage IBD-related constipation.
Dietary Do’s and Don’ts for IBD Constipation
Crohn’s disease is not caused by specific foods, so there is no one diet recommended for people with Crohn’s disease. However, being mindful of what, when, and how you eat (or don’t) can reduce some symptoms as well as promote healing and lower inflammation.
Making good decisions about how to best nourish your body when you have Crohn’s disease is an important part of managing IBD constipation. Here are some dietary tips that may help you manage your IBD constipation:
- DO get to know your body and the trigger foods that contribute to the onset or worsening of your constipation and other Crohn’s symptoms.
- DO avoid your trigger foods, especially when your symptoms are more severe than usual.
- DO use simpler cooking techniques, such as boiling, grilling, and steaming, which are usually a safer choice than frying.
- DON’T overindulge in rich or fatty foods.
- DO increase your water intake, which can help soften stool and make them easier to pass.
- DON’T drink too much caffeine or alcohol, which can be dehydrating.
- DO consider adding more fiber to your diet, which can bulk stools — but don’t make any major changes before speaking with your doctor.
Get Moving for Better Bowel Movements
Staying physically active can help alleviate IBD constipation. Getting your daily exercise can help bowel movements travel through the colon more quickly and easily, which can increase how often you have a bowel movement and help reduce straining.
With unpredictable flares and variable symptom severity, It may not always be easy or possible to exercise during a Crohn’s disease flare. Listen to your body and to your healthcare providers about doing what you can when you can.
Do What Works Best for YOUR Crohn’s
There’s no one-size-fits-all approach to IBD management. Everyone’s IBD affects them differently. For example, increasing the amount of fiber in your diet is a common and effective recommendation to improve constipation. However, during Crohn’s flare-ups, fiber can make things worse. Talk to your IBD treatment team about the specialized diet and specific exercise regimen that’s best for you and your IBD constipation.
Your best bet is to ensure your diet, nutrition, and other at-home strategies align with and complement the pharmaceutical and medical therapies prescribed to help manage your condition. Keep the healthcare professionals who are treating your IBD in the loop as to your diet and making any changes. It’s especially important that you talk to your IBD team or dietician in advance of any dietary changes if you have a stricture.