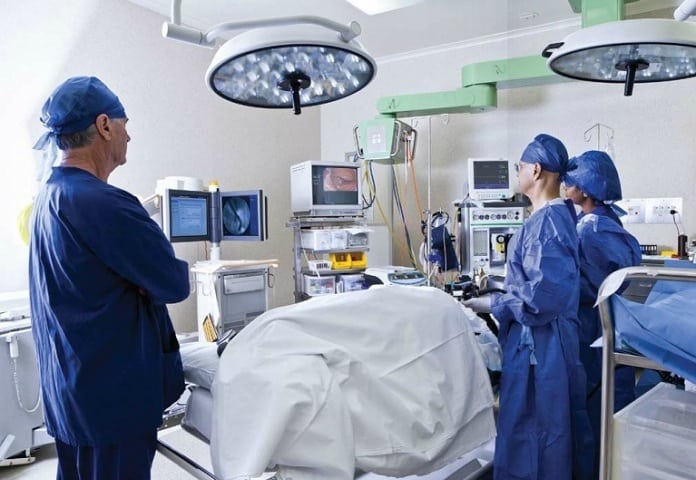
Professor Jacques Marescaux, France, has revolutionized surgery and continues to push the envelope with unprecedented research and training ideas. He believes that hybrid ORs and augmented reality in surgery can improve patient care in the future.
In his recent interview for Siemens Magazine, Marescauz answers few of the very interesting question on Hybrid operating rooms and how is it beneficial for both Patients and Surgeons.
How would you define a hybrid operating room?
Marescaux: You always have a treatment to propose to your patient. Especially in the case of cancer.
We can propose flexible endoscopy, laparoscopic surgery, or interventional radiology. During the operation, surgeons want every possibility to take a closer look inside the patient. Using flexible endoscopy plus surgery, or flexible endoscopy plus 3D image guidance, or interventional radiology plus surgery – that is the idea of the hybrid operating room.
How can we optimize patient care in the future?
Marescaux: One core topic in optimizing patient care is the availability of all patient data from before, during, and after surgery, along with the option of combining this data. Several projects are underway that aim to superpose image data from different imaging modalities. The fusion of image data from an endoscopic camera with DynaCT data, and the fusion of ultrasound images with preoperative CT data are both particularly valuable for minimally invasive procedures.

How will surgery evolve from now?
Marescaux: A few years ago, all the companies developing imaging technology were focusing on the radiology department. Today, it is totally different. Surgeons want to look at all the details of the picture. They no longer depend on the radiologist’s interpretation.
For surgeons, the Artis zeego is a fantastic tool. You have everything you want in real time. But in the future, many surgeons still might not have access to a hybrid room. So they will need to have at least an intraoperative ultrasound system – that will be a good first step. 
What is the role of 3D patient data in that respect?
Marescaux: Virtual reality is one of our institute’s most important tools. It translates real data into digital data, thus allowing us to turn a medical scan into a virtual 3D clone of the patient. The surgeon can then prepare the procedure on the patient’s virtual clone, as these simulations are becoming increasingly realistic.
During the intervention, augmented reality provides a transparent view that should soon allow for the automation of complex surgical movements. This automation will only be possible with developments in the field of surgical robotics.
What opportunities do you see for augmented reality?
Marescaux: To me, augmented reality is the most important improvement for treating patients. One example is complex pelvic surgery, in which surgeons must see the different structures they have to preserve: the urethra, the vessels, and the nerves. In some complex cases, it is impossible to see these three elements. Therefore, we want to have the best image of each structure before the operation.
The concept of augmented reality makes everything transparent. We need to have an intraoperative imaging system that allows us to see all details, even if the organ moves. I’m sure that if we can show that it is an additional benefit for both the patient and the surgeon, it will be mandatory for a hospital to have a hybrid OR. What we have to prove now is its efficiency.
Can you give us an example of how you could prove that efficiency?
Marescaux: Today, a lot of money is still paid out in the event of complications. If we prove that a surgeon has a better view during the operation and that we can thus decrease the complication rate, then paying two or three million euros for a hybrid room is not too much. You will never be the “gold standard” in the future without this new OR concept.
What advice would you give to decision-makers planning an operating room?
Marescaux: The most important thing is to have enough space for all the devices and to give the team access to the patient. It is impossible to know what kind of equipment we will need for each surgical discipline in the future. But for general surgeons, it is important to collaborate with several disciplines on the same platform. If you can perform several steps in one operation, you don’t need two or three anesthesias for the patient.
What skills will surgeons of the future need?
Marescaux: In the USA, there is a lot of specialization, but the majority of surgeons are generalists working in smaller hospitals. I think that surgeons in Europe are more specialized today. One example is that we have “hepatobiliary surgeons” working with surgeons who only do transplants. And the future will probably bring even more specialization.

So what will be the real challenge?
Marescaux: All surgeons like new technologies and the operating room of tomorrow, with all its robotics, will look like the cockpit of an airplane. You will have the robotic system, the 3D visualization, and a lot of screens.
You will push the button and the technology will work for you. It will be very easy. But it will be a challenge for surgeons to know everything about radiation protection. Today, surgeons don’t have enough knowledge of radiation. We want to organize courses to help them understand how best to manage the new kind of OR WeBSurg is a platform for that.
To what extent do robots change operating rooms?
Marescaux: We are still in the prehistory of robotics. At the moment, the robot just improves a surgeon’s abilities. Sure, it is more precise, but that is really just peanuts. However, there is another advantage that will change everything: A robot interface can analyze 1,000 signals per second. When you combine the preoperative image and 3D image guidance with the skill of the surgeon, it will be a huge benefit for the patient.
So are we on the way to the ideal operation?
Marescaux: Today, the 3D image that we take from the CT scan gives us the option of doing the operation before the operation. It is like producing a movie. You do one minute of the operation, then you stop. Then you do another minute, stop again, and then cut the best parts together. The mixture of the imaging and the abilities of the robotic system could really lead to the ideal operation. Maybe we will have automatic surgery in 20 or 30 years time.
What is your wish for the future of surgery?
Marescaux: The real success for surgery will be the day when you really don’t need surgery anymore in some cases. My wish is that imaging progresses and that targeted therapy continues to develop.