Key Takeaways:
- AI significantly enhances clinical accuracy in diagnostics by leveraging advanced algorithms for image analysis and pattern recognition.
- AI powered diagnostics lead to earlier and more precise disease detection, enabling timely interventions and improved patient outcomes.
- These tools augment, rather than replace, human expertise, providing clinicians with robust data-driven clinical decisions and reducing diagnostic variability.
- The integration of diagnostic AI tools across various medical specialties is streamlining workflows and optimizing resource allocation.
- While challenges like data privacy and bias exist, the continuous evolution of healthcare machine learning promises a future of increasingly personalized and predictive diagnostics.
In the intricate world of medicine, diagnostic precision stands as the bedrock of effective treatment and positive patient outcomes. For generations, this precision has relied heavily on the acute observation, extensive training, and cumulative experience of medical professionals. However, a profound transformation is underway, ushering in an era where AI powered diagnostics improving clinical accuracy is not just a concept, but a tangible reality reshaping the healthcare landscape. This technological revolution, driven by sophisticated algorithms and vast datasets, promises a future where diseases are identified earlier, diagnoses are more reliable, and patient care becomes inherently more personalized and effective. The integration of artificial intelligence into diagnostic pathways represents a monumental leap, addressing historical challenges and setting new benchmarks for efficiency and reliability in clinical practice. At HHM Global, we observe that AI-powered diagnostics are rapidly redefining the standards of clinical accuracy and operational efficiency across healthcare systems. As providers increasingly embrace data-driven innovation, AI is becoming central to enabling faster, more reliable, and patient-centric diagnostic pathways.
The Paradigm Shift: From Human Interpretation to Augmented Intelligence
For centuries, diagnostic medicine has evolved through incremental advancements, from the rudimentary examination of symptoms to sophisticated imaging techniques. Yet, even with these advancements, human interpretation, with its inherent subjectivity and susceptibility to fatigue, has remained a critical variable. The introduction of AI in healthcare, particularly in diagnostics, signifies a fundamental paradigm shift. It’s not about replacing human intellect but augmenting it, providing clinicians with an intelligent assistant capable of processing information at speeds and scales previously unimaginable. This augmentation leads directly to enhanced clinical accuracy, providing a safety net and a powerful magnifying glass for practitioners.
The Role of Medical Image Analysis with AI
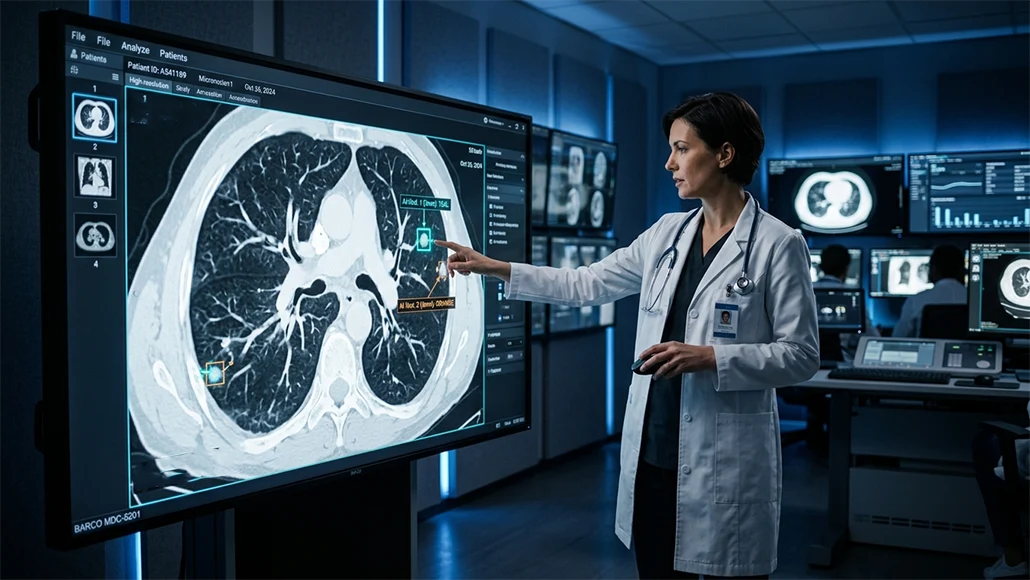
One of the most immediate and impactful applications of AI in diagnostics is in medical image analysis. From X-rays and CT scans to MRIs and microscopic pathology slides, medical imaging generates colossal volumes of data. Traditionally, radiologists and pathologists meticulously scrutinize these images for subtle anomalies. This process is highly demanding and time-consuming. AI algorithms, particularly those leveraging deep learning, are trained on millions of annotated images, enabling them to identify patterns, classify lesions, and even quantify disease progression with astonishing precision. They can detect minute changes that might escape the human eye, or process an entire study in a fraction of the time it would take a human, thereby dramatically enhancing the efficiency and reliability of diagnosis. For example, AI can rapidly screen for early signs of diabetic retinopathy in retinal scans or detect nascent tumors in mammograms, significantly improving the chances of successful intervention.
Precision and Speed: The Hallmarks of AI-Driven Diagnostics
The transformative power of AI powered diagnostics is perhaps best encapsulated by its ability to deliver both unparalleled precision and remarkable speed. These two factors are critically important in clinical settings, where every minute can count and the smallest diagnostic error can have significant consequences for patient health. The relentless processing power of AI systems, combined with their capacity for continuous learning, ensures that diagnostic conclusions are not only swift but also consistently accurate.
Early Disease Detection Through Predictive Analytics
One of the most compelling advantages of AI powered diagnostics improving clinical accuracy lies in its capacity for early disease detection. AI models can analyze a myriad of patient data – from genetic markers and lifestyle information to subtle physiological changes and routine lab results – to identify individuals at high risk for developing certain conditions long before symptoms manifest. This predictive capability extends to analyzing complex patterns in medical images that might indicate the earliest stages of diseases like cancer, Alzheimer’s, or cardiovascular conditions. By identifying these preclinical indicators, AI facilitates proactive intervention strategies, allowing for treatments to begin when they are most effective, often leading to better prognoses and significantly improved quality of life for patients. This shift from reactive to proactive care is a monumental step forward in preventive medicine.
Overcoming Human Limitations and Reducing Variability
Human experts, despite their vast knowledge and experience, are subject to inherent limitations such as fatigue, cognitive biases, and variations in expertise. These factors can lead to inconsistencies in diagnosis. AI, however, operates with unwavering objectivity and consistency. Once trained, a diagnostic AI tool will apply the same rigorous analytical framework to every case, eliminating subjective interpretation and significantly reducing diagnostic variability across different practitioners or institutions. This standardization of diagnostic quality ensures that all patients receive the same high level of scrutiny, regardless of where or by whom their diagnosis is performed, bolstering confidence in the overall healthcare system.
How AI Powered Diagnostics Improving Clinical Accuracy Works: A Technical Glimpse
Understanding the mechanisms behind AI powered diagnostics improving clinical accuracy offers insight into its robustness. At its core, AI in diagnostics leverages sophisticated computational models to identify patterns and make predictions from vast, complex datasets. These models are not simply programmed with rules but learn from examples, much like the human brain, but on an exponentially larger scale.
Machine Learning and Deep Learning in Healthcare
The backbone of modern diagnostic AI lies in healthcare machine learning, particularly deep learning. Deep learning models, often structured as artificial neural networks, are capable of learning complex representations from raw data. For instance, in radiology, a deep learning algorithm might be fed millions of chest X-rays, some labeled as “normal” and others as containing specific pathologies like pneumonia or lung nodules. Through iterative training, the network learns to identify the intricate visual features associated with each diagnosis. This process allows the AI to discover subtle correlations and patterns that might not be immediately obvious to a human observer, making it exceptionally powerful for tasks like image classification, object detection, and segmentation within medical scans.
Integrating Diagnostic AI Tools into Existing Workflows
The practical utility of AI powered diagnostics hinges on its seamless integration into existing clinical workflows. Hospitals and clinics are already equipped with Picture Archiving and Communication Systems (PACS) for images and Electronic Health Record (EHR) systems for patient data. Modern diagnostic AI tools are designed to integrate directly with these platforms. For example, an AI algorithm analyzing a CT scan for a suspected stroke can automatically flag critical findings and highlight areas of concern directly on the image, notifying the radiologist immediately. This integration not only streamlines the diagnostic process but also ensures that AI-derived insights are readily available to clinicians at the point of care, becoming an indispensable part of the decision-making process without requiring disruptive changes to established routines.
Impact Across Specialties: Diverse Applications of AI in Healthcare Diagnostics
The versatility of AI powered diagnostics improving clinical accuracy means its impact is not confined to a single medical discipline but extends across a broad spectrum of specialties, enhancing diagnostic capabilities in myriad ways.
Radiology and Pathology: The Forefront of AI Adoption
Radiology and pathology are arguably the trailblazers in adopting AI for diagnostics. In radiology, AI assists in detecting subtle lesions in mammograms that could indicate early-stage breast cancer, identifying small polyps in colonoscopies, or flagging acute abnormalities like intracranial hemorrhages in emergency scans. For pathologists, AI can analyze vast tissue samples, automating cell counting, identifying cancerous cells, and even predicting tumor aggressiveness from microscopic images. This not only expedites the diagnostic process but also provides a second, highly reliable opinion, significantly boosting the confidence in the final diagnosis. The integration of these diagnostic AI tools allows specialists to focus their expertise on the most complex cases, optimizing their time and reducing burnout.
Cardiology, Oncology, and Beyond
Beyond imaging, AI is making significant strides in other critical areas. In cardiology, AI algorithms analyze ECGs to detect arrhythmias and predict cardiac events, often with greater sensitivity than traditional methods. In oncology, AI assists in tumor classification, staging, and even predicting treatment response based on genomic data and patient characteristics, paving the way for truly personalized cancer therapy. Furthermore, AI is being applied in ophthalmology for glaucoma detection, in dermatology for skin lesion analysis, and in gastroenterology for endoscopy video review. The widespread adoption across these diverse fields underscores the universal applicability and profound benefits of AI powered diagnostics improving clinical accuracy.
The Imperative of Data-Driven Clinical Decisions
Ultimately, the goal of incorporating AI into diagnostics is to empower clinicians with the most comprehensive and reliable information possible, facilitating data-driven clinical decisions. This means transforming raw data into actionable intelligence that directly informs patient management.
From Raw Data to Actionable Intelligence
Medical data is notoriously complex and often fragmented. AI excels at synthesizing vast amounts of disparate information from genetic sequences and imaging results to lab values and patient history and identifying meaningful correlations that might be invisible to human analysis. This capability allows AI to generate clear, concise insights and even suggest potential diagnoses or treatment pathways. Instead of presenting clinicians with a deluge of raw numbers, AI delivers refined, actionable intelligence, supporting more informed and confident decisions. This crucial function helps reduce diagnostic errors and ensures that therapeutic strategies are optimally tailored to each patient’s unique profile.
Enhancing Physician Capabilities, Not Replacing Them
It is crucial to emphasize that AI powered diagnostics are designed to enhance, not replace, the irreplaceable judgment and empathy of healthcare professionals. AI serves as a powerful assistive technology, handling repetitive, high-volume tasks and highlighting critical findings. This allows physicians to dedicate more time to complex problem-solving, patient communication, and delivering compassionate care. The synergy between human intelligence and artificial intelligence creates a superior diagnostic ecosystem, one where the strengths of both are leveraged to their maximum potential. The doctor remains the ultimate decision-maker, but now armed with an unprecedented level of support and insight.
Challenges and Ethical Considerations
While the benefits of AI powered diagnostics improving clinical accuracy are undeniable, the journey is not without its challenges. Addressing these hurdles is vital for the responsible and effective deployment of these powerful technologies. Data privacy, given the sensitive nature of health information, is paramount, requiring robust security protocols and anonymization techniques. Bias in AI models, arising from skewed training data that may not adequately represent diverse populations, is another significant concern that could lead to diagnostic disparities. Furthermore, establishing clear regulatory frameworks for the validation and deployment of medical AI is essential to ensure patient safety and build trust.
The Need for Explainable AI
A key ethical consideration is the “black box” problem, where deep learning models can produce accurate results without transparently showing how they arrived at their conclusions. The medical community requires explainable AI – systems that can provide clear, interpretable reasons for their diagnostic suggestions. This transparency is crucial for clinician trust, for legal accountability, and for continuous learning and refinement of the AI models themselves.
The Future Landscape of Diagnostics with AI
From HHM Global’s perspective, the future of diagnostics is being shaped by the convergence of artificial intelligence, predictive analytics and personalized care models. Healthcare leaders are now focused on scaling AI-driven solutions that not only enhance clinical accuracy but also deliver measurable improvements in patient outcomes and system efficiency. Looking ahead, the trajectory of AI powered diagnostics improving clinical accuracy points towards an increasingly integrated, personalized and predictive healthcare future. The current advancements are merely a prelude to what is yet to come.
Personalized Medicine and Predictive Health
The continued evolution of healthcare machine learning will propel us further into the realm of personalized medicine. AI will enable clinicians to synthesize an individual’s unique genetic makeup, lifestyle data, environmental factors, and real-time physiological monitoring to create highly individualized diagnostic and treatment plans. This level of personalization will move healthcare beyond broad statistical averages to treatments precisely tailored for each patient, maximizing efficacy and minimizing side effects. Moreover, the predictive capabilities of AI will become even more sophisticated, allowing for continuous risk assessment and proactive health management throughout an individual’s lifespan.
Continuous Learning and Evolution of Healthcare Machine Learning Models
Unlike static software, AI models, particularly those leveraging machine learning, are designed to continuously learn and improve. As more data becomes available, and as clinicians provide feedback on AI-generated diagnoses, these models will refine their algorithms, becoming ever more accurate and nuanced. This iterative improvement ensures that AI powered diagnostics will remain at the cutting edge, adapting to new medical knowledge and emerging disease patterns. The future will see these systems not just assisting in diagnosis but also contributing to medical research, identifying new biomarkers, and accelerating drug discovery, further cementing their role as an indispensable component of modern healthcare.
In conclusion, the advent of AI powered diagnostics improving clinical accuracy marks a pivotal moment in healthcare history. By harnessing the immense capabilities of artificial intelligence for tasks like advanced medical image analysis, early disease detection, and facilitating robust data-driven clinical decisions, we are moving towards a future of unprecedented diagnostic precision. While the journey requires careful navigation of ethical and technical challenges, the undeniable benefits ranging from enhanced patient outcomes to more efficient clinical workflows position AI as a foundational technology in shaping a healthier, more reliable, and more equitable healthcare system for generations to come.