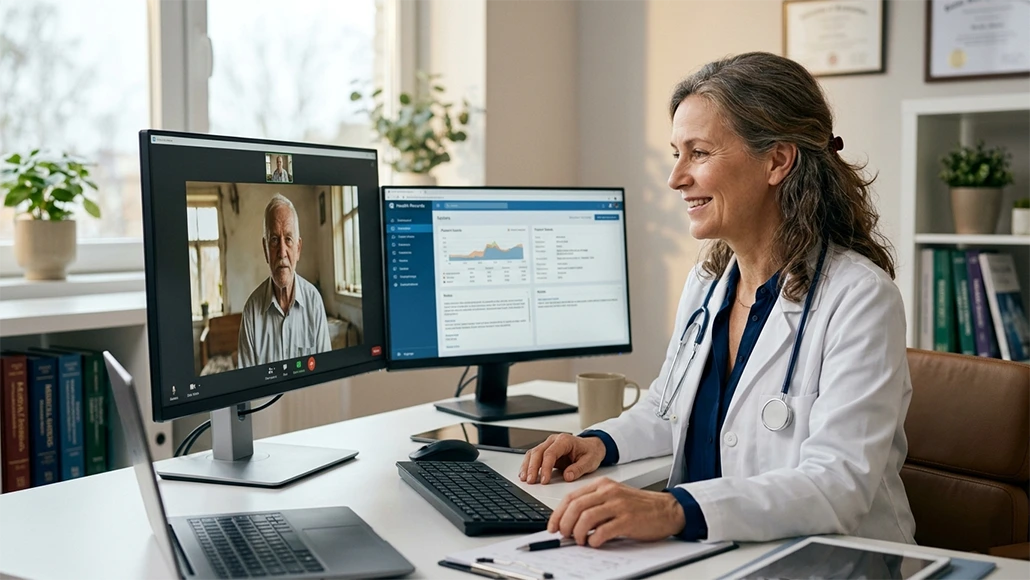
The global healthcare landscape is currently witnessing a tectonic shift, driven by the rapid evolution and integration of digital technology into traditional clinical practices. At the heart of this transformation lies a powerful catalyst: the deployment of sophisticated telemedicine platforms expanding access to remote care for populations that were previously marginalized by geography or socioeconomic constraints. For decades, the primary hurdle in public health has been the physical distance between high-level medical expertise and the patients who need it most. Today, that distance is being collapsed by a web of interconnected devices and secure communication protocols that bring the doctor’s office directly into the patient’s home. This is not merely a matter of convenience; it is a fundamental restructuring of how we define medical presence and patient interaction.
The Architectural Foundation of Modern Telehealth Solutions
To understand how telemedicine platforms expanding access to remote care function so effectively, one must look at the underlying technological architecture that supports them. These platforms are far more than simple video conferencing tools. They are comprehensive ecosystems designed to handle sensitive health data, facilitate real-time diagnostics, and manage complex scheduling workflows across multiple time zones. By integrating electronic health records with secure video interfaces, these systems provide clinicians with a holistic view of a patient’s history while they are engaged in a virtual session. This synergy ensures that the care provided is as informed and precise as any face-to-face encounter. Furthermore, the scalability of these platforms allows healthcare organizations to reach thousands of individuals simultaneously, leveraging cloud computing to ensure that service remains stable even during peak demand periods.
Breaking Down Geographical Barriers in Rural Communities
One of the most profound impacts of telemedicine platforms expanding access to remote care is visible in the revitalization of rural healthcare. In many isolated regions, the shortage of specialists is a chronic issue, often forcing patients to travel for hours to receive basic consultations or follow-up care. The introduction of virtual consultations has effectively eliminated this “distance tax” on health. Patients in remote townships can now connect with top-tier cardiologists, neurologists, or mental health professionals without leaving their local clinics or, in many cases, their own living rooms. This democratization of expertise is critical for early intervention, where the time saved in travel can be the difference between a manageable condition and a life-threatening crisis. By providing a direct link to urban medical centers, these platforms empower rural general practitioners with a support network of specialists, creating a collaborative environment that elevates the standard of care for the entire community.
The Role of Digital Triage in Optimizing Patient Flow
A key component of these systems is the implementation of digital triage, which serves as the first point of contact for many patients entering the virtual care stream. Digital triage utilizes sophisticated algorithms and clinician-supervised questionnaires to assess the severity of a patient’s symptoms before they ever speak to a human provider. This process is essential for telemedicine platforms expanding access to remote care because it ensures that limited medical resources are directed toward those with the highest acuity. Instead of clogging emergency rooms with non-urgent cases, patients can be routed to the appropriate level of care, whether that is a same-day virtual consultation, a prescription refill, or advice for home management. This efficiency not only reduces the burden on physical hospital infrastructure but also minimizes the risk of infectious disease transmission, a lesson that has become permanently etched into the consciousness of the modern medical establishment.
Enhancing Patient Engagement and Longitudinal Care Management
Beyond the immediate crisis or acute consultation, telemedicine platforms expanding access to remote care are proving to be indispensable tools for chronic disease management. Conditions like diabetes, hypertension, and chronic obstructive pulmonary disease require constant monitoring and frequent adjustments to treatment plans. Traditional models of care often see patients falling through the cracks between quarterly appointments. Digital health platforms fill these gaps by facilitating regular, low-friction touchpoints between the patient and their care team. Through integrated wearable devices and mobile health apps, data on vital signs can be transmitted in real-time, allowing clinicians to notice trends and intervene before a complication arises. This proactive approach fosters a stronger sense of partnership between patients and providers, as individuals become more engaged in tracking their own health metrics and understanding the impact of their lifestyle choices.
Overcoming the Challenges of Digital Literacy and Infrastructure
While the promise of telemedicine platforms expanding access to remote care is immense, the transition is not without its hurdles. The “digital divide” remains a significant concern, as those who could benefit most from remote services often lack the high-speed internet or the technical proficiency required to navigate complex software. To address this, forward-thinking developers are focusing on “low-bandwidth” versions of their platforms and designing user interfaces that are intuitive for elderly populations or those with limited tech experience. Moreover, public-private partnerships are increasingly targeting infrastructure improvements in “last-mile” areas, recognizing that broadband access is now a social determinant of health. As these barriers are systematically dismantled, the reach of virtual consultations will continue to expand, ensuring that the benefits of the digital health revolution are shared equitably across all demographic sectors.
The Future of Remote Diagnostics and Integrated Care
Looking forward, the capabilities of telemedicine platforms expanding access to remote care will only grow as they incorporate emerging technologies like artificial intelligence and augmented reality. We are moving toward a future where a virtual consultation might include a remote physical exam assisted by AI-powered diagnostic tools that a patient can use at home. Imagine a scenario where a platform guides a patient through the use of a digital stethoscope or a handheld ultrasound device, with the data interpreted instantly by an AI and verified by a remote physician. This level of integration would further close the gap between virtual and in-person care, making the platform a truly comprehensive medical hub. As these technologies mature, the distinction between “telemedicine” and “medicine” will likely vanish, as digital interaction becomes a standard, seamless part of every patient’s healthcare journey.
Economic Implications and Healthcare Sustainability
From an economic perspective, the shift toward telemedicine platforms expanding access to remote care offers a pathway to more sustainable healthcare spending. By reducing the overhead costs associated with maintaining large physical facilities and decreasing the frequency of unnecessary hospital admissions through better triage and monitoring, these platforms can significantly lower the per-patient cost of care. For insurance providers and national health systems, this represents an opportunity to reallocate funds toward preventative measures and the development of new treatments. For the patient, it means fewer lost wages from travel and time off work, as well as more affordable access to specialized services. In an era where healthcare costs are spiraling upward globally, the efficiency gains provided by digital health tools are not just a luxury but a necessity for the long-term viability of public health systems.
Ethical Considerations and Data Privacy in a Virtual World
As we lean more heavily on telemedicine platforms expanding access to remote care, the ethical implications of data privacy and security take center stage. The transition of medical interactions to the digital realm creates a vast trail of highly personal information that must be protected against breaches and misuse. This requires a robust regulatory framework and a commitment from platform developers to utilize end-to-end encryption and rigorous identity verification. Beyond security, there is the ethical question of maintaining the “human touch” in medicine. While virtual consultations are efficient, the empathetic connection between a doctor and patient is a cornerstone of healing. The most successful telemedicine platforms will be those that use technology to enhance, rather than replace, the human element, providing a space where patients feel heard, understood, and respected despite the digital medium.
Conclusion: A New Era of Inclusive Healthcare
The expansion of telemedicine platforms is fundamentally a story of human ingenuity meeting a critical social need. By leveraging the power of connectivity, we are finally beginning to solve the age-old problem of medical scarcity. Telemedicine platforms expanding access to remote care have proven that quality healthcare is not a fixed point in space but a service that can be delivered wherever a signal can reach. As we continue to refine these tools, improve our digital infrastructure, and integrate virtual care into the broader tapestry of the medical system, we move closer to a world where a person’s zip code no longer determines their life expectancy. The journey toward fully accessible, remote-first healthcare is well underway, and its success will be measured by the millions of lives improved through timely, expert care delivered right where it is needed most.