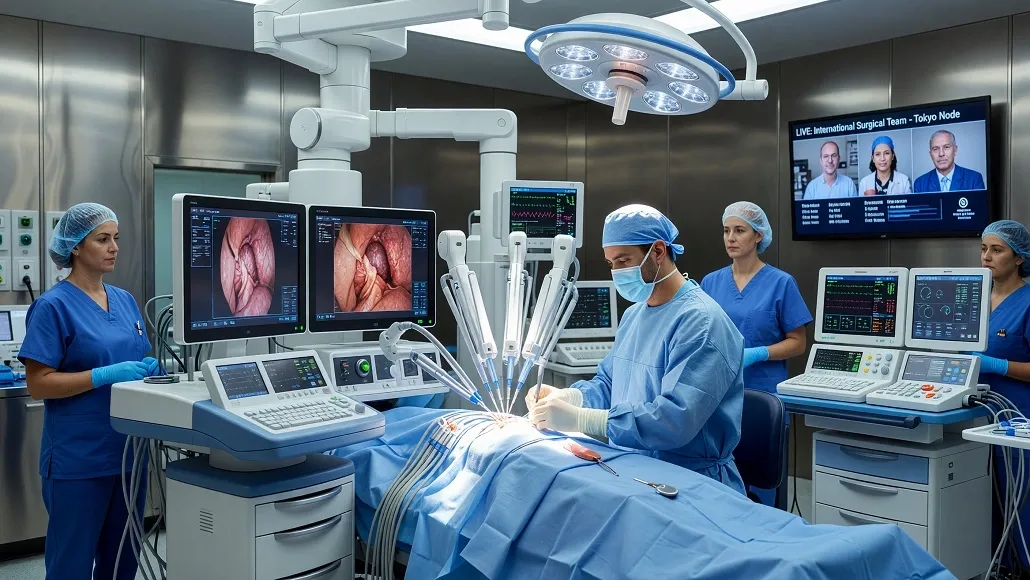
The operating room of the twenty-first century is no longer defined solely by the steady hand of the surgeon but by the seamless integration of advanced mechanical interfaces that extend human capability beyond its natural limits. As we witness how precision surgery robotics minimally invasive care is becoming the gold standard for complex procedures, it is evident that a paradigm shift has occurred. The traditional approach of large incisions and long recovery times is rapidly being replaced by high-precision, robotically-assisted interventions that prioritize patient safety and anatomical integrity. This transition is not merely about using a new tool; it is about fundamentally re-engineering the relationship between the surgeon’s intent and the physical execution of a procedure.
The Technological Foundation of Modern Robotic Surgery
At the heart of this revolution is robotic surgery, a field that has evolved from experimental prototypes to sophisticated multi-arm systems capable of maneuvers that the human wrist simply cannot replicate. Modern surgical automation relies on a combination of high-definition 3D visualization and tremor-filtration software. When a surgeon operates from a console, their movements are translated into precise, micro-scaled actions by the robotic instruments inside the patient’s body. This elimination of natural hand tremors is a cornerstone of precision surgery technology, allowing for sutures and dissections in delicate areas such as the prostate, heart, or brain with a level of accuracy that was previously unimaginable. The result is a significant reduction in collateral tissue damage, which is the primary driver of postoperative pain and inflammation.
Advancing the Scope of Minimally Invasive Robotics
The drive toward minimally invasive robotics has been fueled by the desire to reduce the physical trauma associated with surgery. By utilizing small ports often no larger than a dime surgeons can access internal organs without the need for extensive muscular retraction. This approach is particularly beneficial in oncology, where the precise removal of a tumor while sparing healthy surrounding tissue is the ultimate goal. Advanced surgical systems now incorporate haptic feedback, a technology that allows the surgeon to “feel” the resistance of tissues through the robotic controls. This tactile data, combined with 10x magnification of the surgical site, provides a comprehensive sensory experience that enhances the surgeon’s decision-making process in real-time. The ability to distinguish between a blood vessel and a nerve fiber with such clarity is what defines the new era of precision.
Impact on Patient Recovery and Hospital Resources
The benefits of precision surgery robotics minimally invasive care extend far beyond the operating table and into the recovery ward. Patients who undergo robotically-assisted procedures often experience significantly shorter hospital stays compared to those who have traditional open surgery. For a hospital, this means increased bed turnover and a more efficient allocation of clinical staff. From the patient’s perspective, it translates to a faster return to daily activities, less reliance on opioid pain medication, and smaller, less visible scarring. This improvement in patient outcomes is a primary reason why healthcare providers are increasingly investing in these high-cap systems despite their substantial initial costs. The long-term savings associated with reduced complications and readmissions often outweigh the upfront expenditure, making it a sound strategic move for forward-thinking medical institutions.
In addition to shorter stays, the risk of postoperative infection is markedly lower in minimally invasive robotic procedures. Smaller incisions mean less exposure of internal tissues to the environment, and the precision of the robotic arms reduces the likelihood of accidental tissue trauma that can lead to inflammatory responses. This safety profile is especially critical for elderly patients or those with comorbid conditions who might not tolerate the physiological stress of traditional open surgery. By expanding the population of patients who can safely undergo complex surgical interventions, robotics is effectively democratizing high-quality surgical care and ensuring that age or frailty are no longer absolute barriers to treatment.
Surgical Automation and the Role of Artificial Intelligence
As we look deeper into the mechanics of advanced surgical systems, the integration of artificial intelligence (AI) is beginning to play a pivotal role. Current systems are moving beyond simple teleoperation toward semi-autonomous assistance. For example, AI algorithms can now analyze live video feeds to identify anatomical landmarks and warn the surgeon if they are approaching a critical structure. In some instances, surgical automation can assist with repetitive tasks like suturing or camera positioning, allowing the lead surgeon to focus entirely on the most complex aspects of the operation. This synergy between human expertise and machine intelligence is the hallmark of the next generation of robotic surgery, where the system acts as a co-pilot rather than just a passive instrument.
Furthermore, machine learning models are being trained on thousands of hours of surgical footage to identify the “best practices” for specific maneuvers. This “collective intelligence” can be made available to surgeons in real-time, providing them with guidance and suggestions based on the outcomes of thousands of previous procedures. This level of data-driven support is transforming surgery from an individual craft into a standardized, evidence-based science. As these AI models continue to evolve, we can expect to see even higher levels of automation, potentially allowing robots to perform entire segments of a procedure with minimal human oversight, thereby increasing throughput and reducing the variability of outcomes between different surgeons.
Enhancing Global Access to Specialized Surgical Care
One of the most profound implications of precision surgery robotics minimally invasive care is the potential for telesurgery. Because the surgeon operates from a digital console, that console does not necessarily need to be in the same room or even the same city as the patient. While latency issues in telecommunications have historically been a barrier, the rollout of high-speed 5G and satellite networks is making remote robotic surgery a tangible possibility. This technology could provide rural or underserved areas with access to world-class specialists without the need for patient transport. A specialist in London could potentially assist a surgery in a remote village, bringing elite surgical precision to populations that have traditionally been left behind by medical progress.
This global connectivity also facilitates collaborative surgery, where multiple experts from different parts of the world can log into the same surgical console to assist on a particularly complex case. This “virtual scrub-in” allows for a level of peer review and expert consultation that was previously impossible. For developing nations, this could mean the ability to provide advanced cardiac or neurological procedures that were previously unavailable due to a lack of local specialists. By decoupling the surgeon’s physical location from the patient’s bedside, robotics is paving the way for a more equitable global healthcare landscape where geography is no longer a determinant of surgical quality.
Training the Next Generation of Robotic Surgeons
The shift toward robotic systems has also necessitated a complete overhaul of surgical education. Trainees now spend hundreds of hours on high-fidelity simulators before they ever touch a patient. These virtual environments allow them to practice complex scenarios and manage potential complications in a risk-free setting. This method of training is far more efficient than the traditional “see one, do one, teach one” model of the past. Robotic surgery platforms also allow for the recording and analysis of every movement made during a procedure. This data can be used to provide objective feedback to surgeons, helping them refine their technique and ensure that every patient receives the highest possible standard of care.
Beyond individual skill development, these platforms allow for the standardization of surgical curriculum across different institutions. A resident in Tokyo can be evaluated using the same metrics as a fellow in New York, ensuring a universal baseline of competency. The ability to replay a surgery in 3D and analyze the precision of each movement provides an unprecedented level of insight into the surgical process. This “black box” approach to surgery similar to that used in aviation is driving a culture of continuous improvement and safety that will benefit the entire medical community. As simulators become even more realistic, incorporating patient-specific anatomical data, surgeons will be able to “rehearse” a specific patient’s operation multiple times before entering the actual operating room.
Navigating the Ethical and Financial Landscape
The widespread implementation of precision surgery robotics minimally invasive care is not without its complexities. The high cost of purchasing and maintaining these systems, along with the expensive disposable instruments required for each procedure, creates a divide between well-funded private hospitals and public health systems. There are also ongoing debates regarding the ethical implications of increasing automation. As systems become more autonomous, who is responsible if a mechanical failure or an algorithmic error occurs? These questions require robust legal and ethical frameworks to ensure that patient safety remains the paramount priority.
Furthermore, the industry must work toward creating more affordable, modular robotic platforms that can be adopted by a wider range of healthcare providers globally. Competition between different manufacturers is already starting to drive down prices and spur innovation in new types of robotic interfaces, such as flexible, single-port systems that can navigate natural orifices. As the market matures, the focus will likely shift from purely technical capabilities to the overall value proposition balancing cost, clinical outcomes, and patient experience. Ensuring that the benefits of robotic surgery are available to the many, rather than the few, is the next great challenge for the medical technology industry.
Conclusion: The Future of the Robotic Operating Suite
As precision surgery enters this new era with robotics, we are witnessing the maturation of a technology that was once the stuff of science fiction. The integration of precision, visualization, and intelligence is creating a safer and more effective surgical environment. While challenges remain regarding cost and access, the trajectory is clear: the future of surgery is robotic. By continuing to refine these systems and expanding their capabilities, the medical community is ensuring that patients everywhere can benefit from the highest levels of accuracy and care.
In the coming decades, the operating room will likely become an even more integrated digital ecosystem, where the robot, the imaging systems, and the patient’s electronic records are all part of a single, intelligent network. This will allow for real-time adjustments to the surgical plan based on intraoperative data, further reducing the risk of complications. The synergy of human intuition and mechanical perfection is not just changing surgery; it is redefining what it means to heal. We are moving toward a future where “perfect” surgery is the standard expectation, and where the limitations of the human hand are no longer the limitations of medical science.